“There’s no reason to believe that the virus has run out of room, genetically.”
— Kartik Chandran, Professor of Microbiology and Immunology, Albert Einstein College of Medicine, NYC
###
As we reel from Covid — about 2,000 new cases a week in Humboldt County, mostly the Omicron strain — many of us have four concerns, to which the experts I’ve been following are mostly united in their responses, as follows:
- Will a completely new variant appear this year? Dunno, but almost certainly
- How contagious will it be (i.e. how quickly will it spread)? Dunno
- How well will it evade our immune system, whether or not we’re vaccinated? Dunno
- How virulent (severe) will it be? Dunno
Much of the uncertainly about future of Covid stems from the Omicron variant, which came out of left field, blindsiding the experts. This diagram, in which Covid variants are scaled radially by genetic distance, shows that Omicron is radically different from previous strains of the virus.
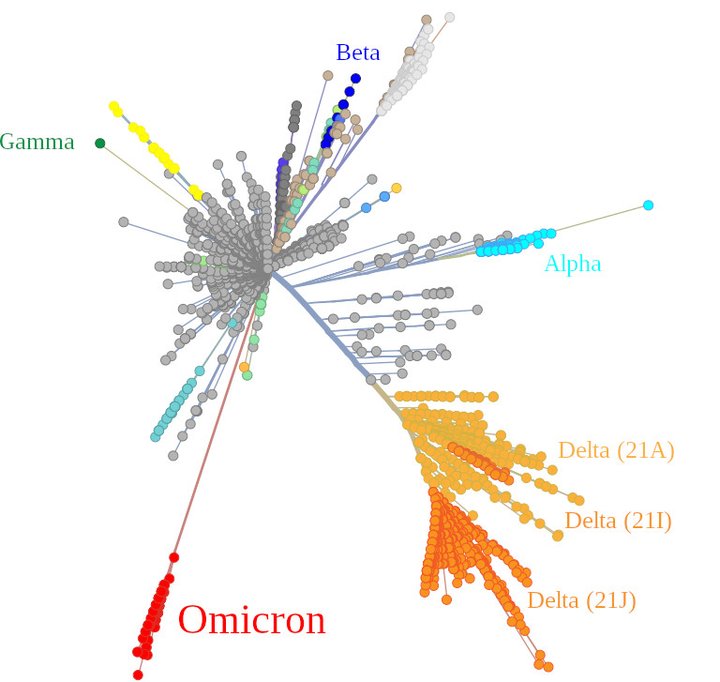
Graphic: Soupvector, via Wikimedia. Creative Commons license.
Conventional wisdom conflates contagiousness, or transmissibility, with mild symptoms, that is, if you’re infected but either don’t know it (very mild symptoms) or think you’ve just got a bout of flu, you’re likely to keep working and hanging with family and friends — thus rapidly and efficiently spreading the virus. The Omicron variant, for instance, grows more easily in the upper airways (70 times faster than the Delta variant) but less easily in the lungs. Meaning that it generally causes less severe disease than Delta, while being super-contagious. So you might expect a pattern in which viruses evolve to become less virulent (but more contagious) versions of their earlier selves.
However, the Delta variant blew conventional wisdom out of the water: it spread more easily than the original Alpha version while doubling Alpha’s risk of hospitalization for unvaccinated people. For that matter, HIV, Ebola and smallpox (the latter now thankfully eliminated) all maintained their severity, despite being long-lived diseases.
So what can we say about the future of Covid-19? In an interview with Live Science, Karen Mossman, Professor of Pathology and Molecular Medicine at McMaster University in Hamilton, Ontario, summed it up like this: “As more and more people become infected and/or vaccinated…they will build up higher levels of immunity against different variants…the overall evolution of SARS-CoV-2 will likely decline, and the pandemic will become endemic.” (Endemic = restricted to certain areas.) At this point though, two years into the pandemic, about 40 percent of the world’s population are unvaccinated. So the virus has plenty of wiggle room to evolve into new and scarier versions.
Finally, you already know you’re at greater risk if you’re not vaccinated, of course, but the degree of that “greater” is worth noting. Nationwide, CDC reports that unvaccinated adults are eight times more likely to be hospitalized with COVID-19 than those who are vaccinated, while locally, according to Humboldt County Public Health, unvaccinated residents are 17 times more likely to be hospitalized with the virus than their vaccinated counterparts.
Do I really need to restate the obvious? Public Health: covidinfo@co.humboldt.ca.us or (707) 441-5000.
CLICK TO MANAGE